The threat of cybercrime is increasing and getting more sophisticated.
The NHS portal scheme is potentially going to give cyber criminals greater access to patient records. We discuss how you...
20 March 2023
Times they are a changing…
It’s not just the clocks going back that we have to worry about. The structure of the NHS is constantly...
4 November 2022
 What if your home was severely damaged due to fire, flood or water leakage?
What if your home was severely damaged due to fire, flood or water leakage?
How does the rising cost of building materials affect homeowners, and why is having a valid Reinstatement Cost Assessment so...
16 August 2022
 Additional protection for your clinical staff
Additional protection for your clinical staff
Whilst State-backed indemnity (CNSGP) will protect NHS work undertaken in respect of clinical negligence, the scope is very basic. Don’t assume...
16 August 2022
 Risk Management- How to avoid the Summertime Blues
Risk Management- How to avoid the Summertime Blues
Our claims department see a number of reoccurring themes when it comes to claims. With experience and the benefit of...
16 August 2022
What is under insurance?
If you have set your cover limits too low or have undervalued your assets, your cover may not adequately meet...
22 July 2022
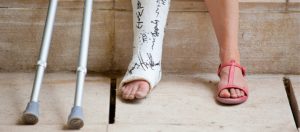 MIAB Locum Insurance
MIAB Locum Insurance
Whilst the NHS provides some reimbursement should a staff member be unable to work, you could still experience an alarming...
13 May 2022
 Primary Care Networks (PCN)- incorporation and insurance considerations
Primary Care Networks (PCN)- incorporation and insurance considerations
The majority of practices who have collaborated have been working under joint contracts for the last 12 – 18 months....
13 May 2022
 Benefact Group
Benefact Group
As you know, we’re a very different type of business. You may not know that we’re owned by a charity,...
26 April 2022
 6 Reasons to have Cyber Insurance
6 Reasons to have Cyber Insurance
Download our flyer today! With cybercrime growing at exponential rates, it has become harder than ever to keep your practice...
19 April 2022
 Are you prepared to weather the storm?
Are you prepared to weather the storm?
Read our tips on how to make a claim. The Met Office have issued a rare RED weather warning as...
18 February 2022
Theft where you least expect it
There are a lot of things to think about when you’re buying a practice, but you don’t expect to have...
25 May 2021
How has Covid-19 impacted cyber security?
It’s a sad fact of life that unscrupulous criminals will use difficult or challenging situations to their own advantage and...
25 May 2021
What is entity cover and why is it important?
Individual indemnity cover may protect you but it won’t protect your business. There are around 14,124 dental practices in the...
25 May 2021
Why is Management Liability Insurance an important consideration
Managers, such as Directors or Officers of a business, have liabilities, statutory duties and responsibilities. Failure to meet your duties,...
24 May 2021
Business Interruption and Supreme Court Verdict (Update)
On 15th January 2021, the Supreme Court delivered its judgment on the Financial Conduct Authority’s (FCA) business interruption test case....
8 February 2021
Business Interruption and Supreme Court Verdict
On 15th January 2021, the Supreme Court delivered its judgment on the Financial Conduct Authority's (FCA) business interruption test case....
22 January 2021
How to survive Christmas
There is no doubt that a ‘Pandemic’ Christmas post lockdown is going to be rather different for many reasons. We...
18 December 2020
Useful links for clients who may be experiencing financial difficulty | COVID 19
We are aware that some of our clients may be experiencing financial difficulty during the current coronavirus pandemic. We are...
5 November 2020
Lorega assistance insurance – expert help when you need it
An add-on benefit that we can offer with your policy is support through specialist firm Lorega. They are a UK...
27 October 2020
Business Emergency Solutions – help is a phone call away
Your practice building is constantly exposed to possible damage, and it’s not just your patients that sometimes need fast emergency...
27 October 2020
Terrorism insurance
The pandemic has provided new opportunities for terrorists and many sources are predicting an impending increase in physical attacks next...
27 October 2020
Bridging the gap in state backed indemnity
During the first wave of the pandemic, GPs were acting as gatekeepers to prevent hospitals being inundated with patient admissions....
12 October 2020
Cyber security in a (big) nutshell
Cyber security is a huge topic, as can be seen from our #CyberSeptember series. Healthcare professionals are faced with so...
29 September 2020
The pandemic effect
Out of the five most likely global risks expected in 2019, two of them were data theft or fraud and...
29 September 2020
Use of IoT (Internet of things) technology leads to greater security risks
There is no doubt that the growing use of mobiles, internet enabled devices and the interconnectedness of devices sharing data...
29 September 2020
Bin Raiders
Cyber criminals are using evermore ingenious and cunning ways to infiltrate systems, so greater vigilance is needed in these challenging...
29 September 2020
Patching up your practice IT
Patches are software updates, a small adjustment to the code, usually released to improve the performance or fix bugs and...
29 September 2020
Data Breaches- Where is the weakest link?
According to a recent Identity Management Institute report (Jan 2020), employee errors cause the most data breach incidents in cyber-attacks....
29 September 2020
 How much do you know about Practice Expenses Insurance
How much do you know about Practice Expenses Insurance
How much do you know about Practice Expenses Insurance? Written by Tristan Lennox-Gentle, Director Practice Expenses Insurance may seem complicated...
24 September 2020
 Practice Insurance & Covid-19 – Update
Practice Insurance & Covid-19 – Update
The Financial Conduct Authority (FCA) brought court proceedings in July 2020 to test how certain business interruption insurance policies respond...
17 September 2020
 REDUCING GP PRESSURE AND ADDING VALUE: PHARMACISTS IN GENERAL PRACTICE
REDUCING GP PRESSURE AND ADDING VALUE: PHARMACISTS IN GENERAL PRACTICE
Reducing GP pressure and adding value: pharmacists in general practice Written by Tristan Lennox-Gentle, Director The delivery of primary care...
9 September 2020
 SURGERY INSURANCE: WHY CHOOSE MIAB?
SURGERY INSURANCE: WHY CHOOSE MIAB?
Surgery Insurance: Why choose MIAB? Written by MIAB's Surgery Insurance Team Running a healthcare practice is unlike most other businesses,...
9 September 2020
 ‘TOP-UP’ LOCUM INSURANCE FROM MIAB COMPLEMENTS NHS SICKNESS REIMBURSEMENT
‘TOP-UP’ LOCUM INSURANCE FROM MIAB COMPLEMENTS NHS SICKNESS REIMBURSEMENT
‘Top-Up’ Locum Insurance from MIAB complements NHS Sickness Reimbursement The General Medical Services (GMS) contract in England for 2018/19 includes...
9 September 2020
 GOVERNMENT INDEMNITY SCHEME FOR GPS – PREPARING FOR CHANGE
GOVERNMENT INDEMNITY SCHEME FOR GPS – PREPARING FOR CHANGE
Government Indemnity Scheme for GPs – Preparing for Change Written by Tristan Lennox-Gentle, Director The announcement of a Government-backed indemnity scheme by...
9 September 2020
 HOW NUDGING TECHNIQUES COULD HELP TO DECREASE THE NUMBER OF DNAS
HOW NUDGING TECHNIQUES COULD HELP TO DECREASE THE NUMBER OF DNAS
How nudging techniques could help to decrease the number of DNAs By Katherine Baterip, Customer Relationship Executive Patients that do...
9 September 2020
 GP FORWARD VIEW – WHAT YOU NEED TO KNOW
GP FORWARD VIEW – WHAT YOU NEED TO KNOW
GP Forward View - What you need to know Written by Jordan Odell, Digital Marketing Executive In April 2016, the...
9 September 2020
 INCOME PROTECTION: KEY CONSIDERATIONS
INCOME PROTECTION: KEY CONSIDERATIONS
Income Protection: Key Considerations Written by Paula Storey, Specialist Protection Insurance Adviser Income Protection is designed to support you if you...
9 September 2020
 MIAB AT PCPA’S ANNUAL MEMBERS CONFERENCE IN MANCHESTER, 11TH OF JULY 2018
MIAB AT PCPA’S ANNUAL MEMBERS CONFERENCE IN MANCHESTER, 11TH OF JULY 2018
MIAB at PCPA's Annual Members Conference in Manchester, 11th of July 2018 The PCPA are hosting their Annual Members Conference...
9 September 2020
 CAN PHARMACISTS AND COMMUNITY PHARMACY RESCUE GENERAL PRACTICE?
CAN PHARMACISTS AND COMMUNITY PHARMACY RESCUE GENERAL PRACTICE?
Can pharmacists and community pharmacy rescue general practice? Pharmacists could play a vital role in primary care and help support...
9 September 2020
 AVERAGE COST OF CLAIMS FOR MIAB’S PRACTICE INSURANCE
AVERAGE COST OF CLAIMS FOR MIAB’S PRACTICE INSURANCE
Average cost of claims for MIAB's Practice Insurance Written by Hannah Wells, Claims Handler Running a medical or healthcare practice...
9 September 2020
 INDEMNITY – WHY CHOOSE MIAB?
INDEMNITY – WHY CHOOSE MIAB?
Indemnity - why choose MIAB? Written by Montrose Bill, Specialist Indemnity Insurance Adviser Protecting you and your business You’ve worked...
9 September 2020
 MIAB ARE DELIGHTED TO ANNOUNCE AN EXCITING NEW PARTNERSHIP WITH INTEGRO
MIAB ARE DELIGHTED TO ANNOUNCE AN EXCITING NEW PARTNERSHIP WITH INTEGRO
MIAB are delighted to announce an exciting new partnership with Integro Offering customers Motor, Household and Travel Insurance. Who are...
9 September 2020
 ALL CHANGE IN THE WORLD OF PRIMARY CARE PROTECTION
ALL CHANGE IN THE WORLD OF PRIMARY CARE PROTECTION
All Change in the World of Primary Care Protection Written by Robert Lynch, Managing Director Medical indemnity protection has become...
9 September 2020
 WHAT’S THE RIGHT LEVEL OF COVER FOR YOU?
WHAT’S THE RIGHT LEVEL OF COVER FOR YOU?
Written by Specialist Adviser, Emily McMillan When it comes to protecting your practice against staff absence, there are several options...
9 September 2020
 INDEMNITY COVER FOR DENTISTS – SOMETHING TO CHEW ON
INDEMNITY COVER FOR DENTISTS – SOMETHING TO CHEW ON
Indemnity Cover for Dentists - something to chew on Written by Andrew North, Director All practicing dentists should understand the...
9 September 2020
 BUSINESS AS (UN)USUAL – GETTING BACK TO NORMAL AFTER A SERIOUS INCIDENT
BUSINESS AS (UN)USUAL – GETTING BACK TO NORMAL AFTER A SERIOUS INCIDENT
Business as (Un)usual - Getting back to normal after a serious incident By Hannah Wells, Claims Handler and Gianni Brancazio,...
9 September 2020
 PERSONAL AND FAMILY INSURANCE – ARE YOU COVERED?
PERSONAL AND FAMILY INSURANCE – ARE YOU COVERED?
Personal and Family Insurance – Are you covered? Written by Specialist Protection Insurance Adviser, Paula Storey Purchasing insurance for your...
9 September 2020
PROFESSIONAL INDEMNITY COVER: MDOS V INSURANCE POLICIES
Professional Indemnity Cover: MDOs v Insurance Policies Written by Andrew North, Director Healthcare professionals are committed to delivering a high...
9 September 2020
 NHS DENTAL RECRUITMENT CRISIS – OVERHEADS PROTECTION WHEN YOU NEED IT MOST
NHS DENTAL RECRUITMENT CRISIS – OVERHEADS PROTECTION WHEN YOU NEED IT MOST
NHS Dental recruitment crisis – Overheads protection when you need it most Written by MIAB's Specialist Business Overheads Insurance Adviser...
9 September 2020
 EMAIL FRAUD – PROTECTING YOUR BUSINESS
EMAIL FRAUD – PROTECTING YOUR BUSINESS
Email Fraud – Protecting your Business By Hannah Wells, Claims Handler Financial Fraud Action UK, which is leading the fight against...
9 September 2020
 THE IMPLICATIONS OF CLAWBACK IN NHS DENTISTRY
THE IMPLICATIONS OF CLAWBACK IN NHS DENTISTRY
Written by Andrew North, Director As a business owner, the ability to forecast your income and outgoings is paramount to...
9 September 2020
 PHARMACIST LOCUM RATES INCREASE
PHARMACIST LOCUM RATES INCREASE
Written by MIAB's Specialist Business Overheads Insurance Adviser Locum rates are a constant battle of supply versus demand, and influenced...
9 September 2020
 PROTECTING YOUR STAFF AND BUSINESS
PROTECTING YOUR STAFF AND BUSINESS
Protecting your staff and business Written by MIAB's Specialist Business Overheads Insurance Adviser, and Paula Storey, Specialist Protection Insurance Adviser....
9 September 2020
 HOW MUCH DO YOU KNOW ABOUT LOCUM INSURANCE?
HOW MUCH DO YOU KNOW ABOUT LOCUM INSURANCE?
How much do you know about Locum Insurance? Written by Anmol Paul, Specialist Locum Insurance Adviser Locum Insurance may seem...
9 September 2020
 HURRICANE GERT SET TO HIT THE UK – WHAT TO DO IN THE EVENT OF A STORM
HURRICANE GERT SET TO HIT THE UK – WHAT TO DO IN THE EVENT OF A STORM
Hurricane Gert set to hit the UK - what to do in the event of a storm Written by Jordan...
9 September 2020
 THE DISCOUNT RATE – WHAT DOES THIS MEAN FOR PERSONAL INJURY PAY-OUTS?
THE DISCOUNT RATE – WHAT DOES THIS MEAN FOR PERSONAL INJURY PAY-OUTS?
The Discount Rate - What does this mean for personal injury pay-outs? Written by Robert Lynch, Managing Director A seemingly...
9 September 2020
 INCOME PROTECTION FOR DENTISTS
INCOME PROTECTION FOR DENTISTS
Income Protection for Dentists Written by Paula Storey, Specialist Protection Insurance Adviser Income Protection Insurance is designed to cover you...
9 September 2020
 INSURANCE CHARITIES AWARENESS WEEK: 17TH – 21ST JUNE
INSURANCE CHARITIES AWARENESS WEEK: 17TH – 21ST JUNE
Insurance Charities Awareness Week: 17th - 21st of June At MIAB, we are once again supporting Insurance Charities Awareness Week!...
9 September 2020
 DENTAL INDEMNITY – YOUR OPTIONS BEYOND DEFENCE ORGANISATIONS
DENTAL INDEMNITY – YOUR OPTIONS BEYOND DEFENCE ORGANISATIONS
Dental Indemnity – Your Options Beyond Defence Organisations Written by Tristan Lennox-Gentle, Director As a Dentist every minute of your...
9 September 2020
 PRACTICE INSURANCE: WHY CHOOSE MIAB?
PRACTICE INSURANCE: WHY CHOOSE MIAB?
Practice Insurance: Why choose MIAB? Written by MIAB's Practice Insurance Team Running a healthcare practice is unlike most other businesses,...
9 September 2020
GREAT FEEDBACK ABOUT OUR POLICY FOR PHARMACISTS IN GENERAL PRACTICE
Great feedback about our policy for Pharmacists in General Practice We value our customer feedback and use it to further...
9 September 2020
 THE UK DENTAL INDUSTRY AND IMPLICATIONS OF A NO-DEAL BREXIT
THE UK DENTAL INDUSTRY AND IMPLICATIONS OF A NO-DEAL BREXIT
Written by MIAB's Specialist Business Overheads Insurance Adviser. Brexit is an ever-evolving enigma with an enormous amount of potential outcomes,...
9 September 2020
 5 POINT GDPR CHECKLIST FOR SMALL BUSINESSES
5 POINT GDPR CHECKLIST FOR SMALL BUSINESSES
5 point GDPR checklist for small businesses Written by Jordan Odell, Digital Marketing Executive The General Data Protection Regulation (GDPR)...
9 September 2020
 AVERAGE COST OF CLAIMS FOR MIAB’S ABSENCE INSURANCE
AVERAGE COST OF CLAIMS FOR MIAB’S ABSENCE INSURANCE
Average cost of claims for MIAB's Absence Insurance Written by Hannah Wells, Claims Handler Absences are unavoidable in any line...
9 September 2020
 STORM DORIS – PROTECTING YOUR BUSINESS
STORM DORIS – PROTECTING YOUR BUSINESS
Storm Doris – Protecting your Business Written by Hannah Wells, Claims Handler Storm Doris has struck Britain today, causing damage...
9 September 2020
 SICKNESS COVER REIMBURSEMENT FOR GPS: IMPACT OF RISING LOCUM COSTS
SICKNESS COVER REIMBURSEMENT FOR GPS: IMPACT OF RISING LOCUM COSTS
Sickness Cover Reimbursement for GPs: Impact of Rising Locum Costs MIAB has been exploring the impact of the changes to sickness cover...
9 September 2020
 IT’S NOW MORE IMPORTANT THAN EVER TO HAVE STRONG LEADERS IN HEALTHCARE
IT’S NOW MORE IMPORTANT THAN EVER TO HAVE STRONG LEADERS IN HEALTHCARE
It's now more important than ever to have strong leaders in healthcare Written by Jordan Odell, Digital Marketing Executive Good...
9 September 2020
 SUPPORTING DOCTORS WITH MENTAL ILLNESS
SUPPORTING DOCTORS WITH MENTAL ILLNESS
Supporting Doctors with Mental Illness Written by Montrose Bill, Specialist Indemnity Insurance Adviser Being a GP has always meant coping...
9 September 2020
 MIAB’S THOUGHTS ON THE ANNOUNCEMENT OF NEW STATE-BACKED INDEMNITY SCHEME
MIAB’S THOUGHTS ON THE ANNOUNCEMENT OF NEW STATE-BACKED INDEMNITY SCHEME
MIAB's Thoughts on the Announcement of new State-backed Indemnity Scheme Written by Robert Lynch, Managing Director The announcement of the...
9 September 2020
 SICKNESS COVER REIMBURSEMENT FOR GPS – FAQS
SICKNESS COVER REIMBURSEMENT FOR GPS – FAQS
ickness cover reimbursement for GPs - FAQs Written by Anmol Paul, Specialist Locum Insurance Adviser The General Medical Services (GMS)...
9 September 2020
 KEY PERSON ABSENCE COVER – PROTECTING YOUR STAFF
KEY PERSON ABSENCE COVER – PROTECTING YOUR STAFF
Key Person Absence Cover - Protecting Your Staff Written by James Pearce and Abby Thynne, Specialist Surgery Insurance Advisers It...
9 September 2020
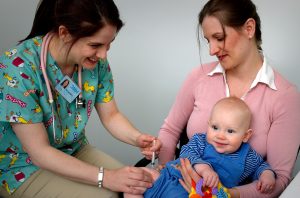 LOSS OF VACCINES – PREVENTION AND WHAT TO DO IN ORDER TO CLAIM
LOSS OF VACCINES – PREVENTION AND WHAT TO DO IN ORDER TO CLAIM
Loss of Vaccines - Prevention and what to do in order to claim Written by MIAB's Claims Handler A loss...
9 September 2020
Extra security for diabetics – Insurer introduces Diabetes Life Cover Written by Paula Storey, Specialist Protection Insurance Adviser At MIAB,...
9 September 2020
 LOCUM INSURANCE TESTIMONIALS
LOCUM INSURANCE TESTIMONIALS
Locum Insurance Testimonials Written by MIAB's Clients We’re delighted to share testimonials from customers about our Locum Insurance. From New...
9 September 2020
 BUSINESS OVERHEADS INSURANCE WITH MIAB
BUSINESS OVERHEADS INSURANCE WITH MIAB
Business Overheads Insurance with MIAB Written by MIAB's Specialist Business Overheads Insurance Adviser. An inevitable challenge business owners face is their...
9 September 2020
 MIND THE GAP – BRIDGING THE DIVIDE BETWEEN NEW MODELS OF CARE AND GOVERNMENT INDEMNITY
MIND THE GAP – BRIDGING THE DIVIDE BETWEEN NEW MODELS OF CARE AND GOVERNMENT INDEMNITY
Mind the gap - Bridging the divide between new models of care and government Indemnity Written by Tristan Lennox-Gentle, Director...
9 September 2020
 ENCOURAGING SELF-CARE WITHIN YOUR PRACTICE CAN LESSEN THE DEMAND FOR MINOR AILMENT APPOINTMENTS
ENCOURAGING SELF-CARE WITHIN YOUR PRACTICE CAN LESSEN THE DEMAND FOR MINOR AILMENT APPOINTMENTS
Encouraging self-care within your practice can lessen the demand for minor ailment appointments Written by Jordan Odell, Digital Marketing Executive...
9 September 2020
 LOCUM INSURANCE: WHY CHOOSE MIAB?
LOCUM INSURANCE: WHY CHOOSE MIAB?
Locum Insurance: Why choose MIAB? Written by Anmol Paul, Specialist Locum Insurance Adviser Protect your business With so much pressure...
9 September 2020
 BEDS & HERTS LMC GP & PRACTICE MANAGER CONFERENCE – FACING THE FUTURE WITH OPTIMISM
BEDS & HERTS LMC GP & PRACTICE MANAGER CONFERENCE – FACING THE FUTURE WITH OPTIMISM
Beds & Herts LMC GP & Practice Manager Conference - Facing the Future with Optimism Beds & Herts LMC are...
9 September 2020
 MIAB ARE PROUD TO SPONSOR PCPA’S CHARITY LONDON TO PARIS BIKE RIDE!
MIAB ARE PROUD TO SPONSOR PCPA’S CHARITY LONDON TO PARIS BIKE RIDE!
You may have been following the news on Twitter or Facebook that the PCPA 'London to Paris' bike ride is quickly approaching! Starting at 10:00am...
9 September 2020
 5 THINGS TO CONSIDER WHEN REVIEWING YOUR DENTAL INDEMNITY COVER
5 THINGS TO CONSIDER WHEN REVIEWING YOUR DENTAL INDEMNITY COVER
5 things to consider when reviewing your Dental Indemnity Cover Written by Tristan Lennox-Gentle, Director As a Dentist you are...
9 September 2020
 MENTAL HEALTH CAN AFFECT ANYONE, INCLUDING HEALTH PROFESSIONALS
MENTAL HEALTH CAN AFFECT ANYONE, INCLUDING HEALTH PROFESSIONALS
Mental health can affect anyone, including health professionals Written by Katherine Baterip, Compliance Support It is estimated that 1 in...
9 September 2020
 STATE-BACKED INDEMNITY FOR ENTITIES: MAXIMISING INCOME
STATE-BACKED INDEMNITY FOR ENTITIES: MAXIMISING INCOME
Written by Tristan Lennox-Gently, Director With just weeks to go until the expected launch of state-backed indemnity, stakeholders including federations and...
9 September 2020
 NHS SICKNESS REIMBURSEMENT: BMA ISSUES ADVICE CORRECTION
NHS SICKNESS REIMBURSEMENT: BMA ISSUES ADVICE CORRECTION
NHS Sickness Reimbursement: BMA issues advice correction Written by Anmol Paul, Specialist Locum Insurance Adviser It has been reported by Pulse that...
9 September 2020
 STATE-BACKED INDEMNITY FOR ENTITIES: MAXIMISING INCOME
STATE-BACKED INDEMNITY FOR ENTITIES: MAXIMISING INCOME
Written by Tristan Lennox-Gently, Director With just weeks to go until the expected launch of state-backed indemnity, stakeholders including federations and...
9 September 2020
 THE COST OF STAFF ABSENCE
THE COST OF STAFF ABSENCE
The Cost of Staff Absence Written by MIAB's Surgery Insurance Team In the current industry climate where according to Pulse one in six posts...
9 September 2020
 THE UK DENTAL INDUSTRY AND IMPLICATIONS OF A NO-DEAL BREXIT
THE UK DENTAL INDUSTRY AND IMPLICATIONS OF A NO-DEAL BREXIT
Written by MIAB's Specialist Business Overheads Insurance Adviser. Brexit is an ever-evolving enigma with an enormous amount of potential outcomes,...
9 September 2020
Primary Care Home Indemnity: Understanding the Considerations
Written by Tristan Lennox-Gentle, Director As part of an innovative and co-ordinated approach to the delivery of primary care, there...
8 September 2020
Protect Your Future By Insuring Your Past
Written by Tristan Lennox-Gentle, Director of MIAB The Clinical Negligence Scheme for General Practice (CNSGP) launched on the 1st of...
8 September 2020

